|
Coronavirus is everyones biggest concern, but it does not mean we will not develop other health problems, such as gastro, appendicitis or injuries. We still need to see the doctor, but at the same time we do not want to expose ourselves to coronavirus, by going out. As a result, doctors have been encouraged to use Telehealth, (Telehealth is where you see a doctor via something like Skype or Facetime). Now you can see your GP by Telehealth under Medicare. As a family physician, I have been using Telehealth for many years. It will never take over from seeing a doctor face to face, but we can achieve a lot using a video consultation. As a doctor I need to gather a lot of information to work out what is wrong with you. If you can give me that information, I can perform a safer consultation via a video. If you have the right tools in your house, you can give me the information that I need and reduce the chance of missing something nasty. These tools have been around for many years and are not high tech. This week, we have created a special edition newsletter to highlight what tools can be used to help your doctor make a safe diagnosis. As mentioned before in this blog, these gadgets should be part of everyones first aid kit, to allow you to always see a doctor from the comfort of your own home, safe from the coronavirus. Online Health ServicesWhether you have the right equipment or not, there are many health services that you can access online. You can see a GP, get a blood test or even an STI check. Click on the button below for more information. For Clinic OwnersIf you are a clinic owner who is setting up a Telehealth service, please click on the link below and cut and paste the URL into an email or sms to be sent to your patients.
You can improve the quality of your Telehealth assessments by informing your patient population how to provide data that can help you make a diagnosis. Please note that your patients will need to be consented to receive communication via this process - Spam Act 2003)
1 Comment
Coronavirus is causing panic. It is a new virus that we know little about. Opinions about the virus can be found on the internet, but who can you really trust? Information changes daily, so how do you keep up to date? We have researched the resources that the specialists are using to inform themselves and their patients and put together a newsletter with access to these resources, that are updated regularly. You need to know this information for the sake of your health and your families. In the best interest of the health of the nation, we are offering this newsletter for free, to clinics to send to their patients. (Just click on the link below, to access the newsletter and then cut and paste the URL into an email that you can send to your patients). If you are planning to travel abroad, click on the link below to see a live tracker of the locations where the virus is present. Created by the John Hopkins University in Baltimore, USA, from credible sources, it lets you know where the infection has broken out.
We are a tech savvy nation. In less than a decade, it is amazing to realise that we all carry around a mini computer in our pockets and at a quick glance at your watch, it can tell you within seconds how many steps you’ve taken, how far you’ve walked, the status of your heart rate and how well you slept last night. This data helps individuals and health professionals to understand how a person functions, and the factors that may be helping - or hindering their health and wellbeing. As a dietitian, much of my role is mostly about exploring and understanding someone’s dietary intake, analysing what nutrients are being met and what potential risks might be on the horizon based on unbalanced or inadequate eating patterns. Although it’s one thing to talk and prescribe nutrition, it’s another thing to teach someone what happens when we eat food, and the impact this has on their own body. This is where I have experienced and seen the value of Continuous Glucose Monitoring (CGM). Although CGM devices are primarily designed and used by people with Type 1 Diabetes, I have used them with healthy fit individuals, as well as people with Type 2 Diabetes, (especially when the national guidelines changed in 2014 to cease self blood glucose monitoring for those not on insulin).
CGM devices provide a wonderful insight into a person’s week of blood glucose levels (BGL), based on their daily activities and eating habits. I have used the Medtronic Guardian Connect which relays real-time data to the individual’s phone, and other options such as the Libre Freestyle also have similar technology. Instead of the individual investing in a device, I provide it as a week-long window of data collection and a chance for my clients to really understand how their food choices impact their bodily systems. The ability to see this instant feedback puts their health and nutrition front of centre and provides a unique opportunity to discuss what happened in a course of 6-14 days. The blood glucose level graph, alongside a food diary allows them to connect the dots when they see when they have eaten in excess or too frequently or too late at night. It also helps to educate people about the effects of glycaemic index of carbohydrates, combinations of macronutrients in a meal (high fibre vs high fat vs high carb) and food cravings based on declining BGLs or timing of meals. For those with insulin resistance, it’s an opportunity to see just how much (and how hard) the body has to work to process their food to return to homeostasis. Fit, healthy individuals also gain insight into the mechanisms of their own body and understand in a tangible way the daily fluctuations and outcomes of food, exercise, sleep and stress has on their health. It’s important to highlight that CGM devices are not for everyone; it is a relatively complex feedback system that requires some base level of health knowledge. It also needs to be noted that viewing BGLs alone is only one part of the story, and measuring insulin levels in parallel would be ultimately provide an even clearer picture of someone’s hormone regulation. I guess we will have to wait and see. But for now, I hope that CGM will become more accessible (and perhaps more affordable) over time as it undoubtedly provides health professionals the invaluable access into a person’s lifestyle habits at home as well as the ability for individuals to grasp a concept that otherwise would be completely foreign to them. Article written by Carla Johnson Dietitian at The Nutrition Circle For more information on The Nutrition Circle, click here Disclaimer: This text does not serve as medical advice or an endorsement of a particular product but serves as an example of how technology can improve healthcare. If you have any questions, seek advice from your doctor. Technology has many roles in healthcare. For it to succeed, the infrastructure needs to be in place to enable the flow of information. We are grateful to have had the opportunity to talk to one of the world's leading experts in healthcare data technology, about how you as a patient can position yourself, to benefit from the changes taking place.
Hello Grahame and thank you for giving us the time to talk about what you are trying to achieve. Can you tell us about your professional background, personal story and how you got involved in healthcare? I was born in Australia but grew up in New Zealand. I graduated with a degree in Biochemistry and Botany with a plan to work on improving plant crop yields but first I decided to have a holiday in Australia. I quickly ran out of money, and was very lucky to get a job in a hospital laboratory doing clinical tests. I realised that healthcare was where I belonged, and I’ve been in it ever since. Over the last 30 years, I’ve worked as a laboratory technician, a medical researcher, a developer of healthcare software, a healthcare IT product manager, and I’ve been a consultant to several national programs and many other software makers to help them exchange and use information across the healthcare system. Given your extensive experience and knowledge in healthcare globally, what would you say the biggest problem in healthcare is today? We have a system where each healthcare provider has a laser focus on best practice with regard to effectiveness and safety for the care that they provide, and I think that we’re well served from that perspective. But no one is accountable for overall outcome of patients in the same way. If a patient has a chronic problem, and especially if they have more than one, the different parts of the healthcare system don’t coordinate well with each other, and patients can easily fall into the gaps. I see that mental health is a particularly problematic area. That’s true both in terms of organising healthcare - making appointments etc, but also true with regard to bigger issues like what your medications and treatment should be, and what the care plan is trying to achieve. Patients often end up managing this contention between different care providers themselves, and I think that in general, they’re the least well informed about the choices they end up having to make. Around the world, people are obsessed with how healthcare is paid for - and that’s a real challenge because as a society we can’t afford all the healthcare that we would like. How we choose to ration healthcare says a lot about who we are as a culture. But I think that right now, there’s still plenty of improvements to be made in how we care for individual patients, and we need to focus on that problem. What have you worked on to help solve it? There’s lots of reasons why the different parts of the system don’t work well together, and lots of people working on those parts. I’m focused on one part, one contributing factor: how difficult (=costly) it is to make information about a patient available in the right place, at the right time, and in the right way. And when information isn’t available, and it takes too long to get it, care providers don’t have time to talk to each other. So my focus is to improve the overall way that we can share information. That means technical standards, through the international standards process. The standards are deeply technical, and process is very arcane, and people find it hard to relate to, and to see the benefit. But the benefits are very real – for example, the things that smart phones can do are built on top of similar information exchange standards. People’s eyes glaze over when I try to explain this, but it’s real, and those of us who work on the standards strongly believe that we’re making a real difference. But we also know that it’s indirect; the standards only have any impact when people use them, and build eco-systems on them. So we also work with governments, hospitals, and companies etc about how and why to leverage the standards we are building. Can you explain FHIR in laymen's terms? I’ll give it a try… “FHIR” is the name of the standard we are working on. It’s an open standard, which means that anyone can read the standard and write software that follows it. It describes a way that different software systems can talk to each other about patient’s healthcare - both to find out what the state of health is and to ask each other for services related to the patient’s care. Given that the software represents people and organisations, the information exchange drives the care process - whether that’s administration, medication management, care planning etc. FHIR is very much based on the latest web technology, which means that it’s easier to use for developers, since web technology has taken over the whole world for developers, and there’s tools and skilled programmers everywhere - though for programmers, actually understanding the healthcare eco-system and ethos takes time and really matters. HL7 is an international standards organisation that is responsible for FHIR. Even the name HL7 shows how arcane this is (what on earth does it mean? The answer is meaningful to very few people). But arcane doesn’t mean irrelevant - existing HL7 standards are used by software in almost every healthcare institution in the developed world. Now we’re bringing our old standards into the latest web based world, and covering more of the healthcare process. So why are Apple, Google, Amazon and Microsoft adopting HL7 FHIR standards? These big companies look at the amazing amounts of money spent on healthcare, and think that maybe they should be more active in the space. But it’s a tough area to be in - any software you write has to cover such a broad range of functionality and you have to support it a long time before it becomes profitable. They’ve failed before, and lost lots of money doing it. Kudos to the current healthcare software providers, then - they’re actually pretty good at what they do! Now these big companies think that the standards we are working on will open up the eco-system so that they can focus on doing what they’re good at - whether it’s bringing slick services to consumers, or helping enterprises understand their data - without having to understand all of healthcare and compete with the existing companies around their healthcare solutions. So they're excited about this potential and are adopting HL7 FHIR, and encouraging all the other software providers to do so. What they’re going to do with the standard…. well, we’ll see. Irrespective, from my point of view, their interest is a good validation of our expectation that good information exchange standards have the power to change the world. What do you want to see change in healthcare today? I’m all about people working together. I want to see out healthcare providers being more nimble in this regard, and being more easily able to work in care teams based around the patient, instead of being in institutionally based care teams. Then I want to see doctors make the most of this and welcome the ability to work together more widely, and to be proactive in improving healthcare outcomes, not responding after the fact to problems. How do you see the future of healthcare change in Australia and globally in 5-7 years? The changes we’d like to see are scary for some people. Digital disruption creates winners and losers, and many people are primarily concerned to make sure that they’re not in the losing group. I think that skilled passionate people won’t have to worry about that - we don’t have enough of them whatever happens. But institutions are good at protecting themselves. So I predict that both in Australia and globally, the future of healthcare over that period will be increasingly characterised by fear based responses to digital change, and very different policy choices by different governments while they try to balance between benefits and risks. Eventually, we’ll see what works and governments will start to respond to their voters and do what actually works. Do you have any tips for patients if they want to improve healthcare data transmission between healthcare providers, related services and their health professionals? In the big picture there’s a real prospect that the patient’s interests will come second to big institutional interests. Patients are the ones who are invested in their own outcomes, but they need to say something. So I encourage patients to ask for access to their health records, and to keep and carry a paper summary of their past medical record and what they understand their current treatment plan is, for all their different health issues. This is both good for patients now, and keeps reminding doctors that people do care. I think that patient’s should experiment with digital tools for collating this information. On the other hand, patients should realise that there’s a long way to go before they can have all their healthcare records on their phone or somewhere of their choice, and that they and the healthcare system can use their own single record to build better ways to provide healthcare. So be… patient… about this. It’s going to take years to work this out. I’m truly sorry if you don’t have years, and I know many people who don’t, sadly - we’re working as hard as we can at the standards level, but there’s a long way to go and a lot of change to make yet. Note that here in Australia, the government is pushing the MyHR system but this is only a little useful for this task so far. I worked on the MyHR and still do, and it’s going on the right direction, but we have a long way to go, and the government isn’t investing enough in pushing this along to go further at the moment. Industry colleagues have often branded you as the private and humble Melbournian "Elon Musk of healthcare". How do you feel about this? Really? That’s strange. There’s thousands of people working on FHIR and standards more generally - writing the standards, or using them to improve software. I might be more visible than many other participants, but I’m just representing their contributions to our shared public treasure (may I do that well). Is that what Elon Musk does? I think no, it’s not the same thing at all. But I am happy to admit that I like living in Melbourne, even given the weather. What do you think of the concept of HealthAide and how it may benefit patients and clinics? I think that It fits naturally into the paradigm that I described above, collecting your data and then using it to improve your health. Over time, it will become more useful as more of the system opens up to provide services in the right way. Grahame, it has been a pleasure talking to you today. Thank you for your time and the opportunity to discuss how you are helping healthcare enter the digital age. About Grahame Grahame Grieve is HL7's Product Director for "FHIR" - the leading healthcare data exchange standard of the future. Grahame has a background in laboratory medicine, software vendor development, clinical research, open source development and has also conceived, developed and sold interoperability and clinical document solutions and products in the Australian market and around the world. Grahame has worked to develop standards and solutions with several US vendor consortiums, and the national programs of Canada, England, Singapore, and Australia. For more information, click here Disclaimer: This text does not serve as medical advice or an endorsement of a particular product but serves as an example of how technology can improve healthcare. If you have any questions, seek advice from your doctor. You need transportation now? Uber.
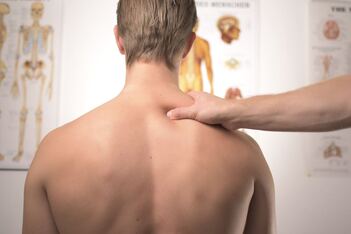
You want to watch the latest movie now? Netflix. You want to see a healthcare practitioner now? Ehm…. In a world where nearly every type of service is available at the tap of an app, it’s surprising there are hardly any apps available to properly manage your own health. Surely, there are fitness apps to follow work outs or apps to book an appointment with a GP or healthcare practitioner. But what if you live remotely and require expert advice from a physiotherapist or exercise physiologist? Or you are jet setting around Europe and need to follow up with your healthcare provider about your rehab exercise program? When we launched Physitrack a few years ago, our aim was to give practitioners and their clients a seamless way of staying in touch and offer complete transparency about the clients’ progress with their home exercise programs. Key in achieving this was the free PhysiApp client apps we developed for iOS, Android and web. Being part of Apple’s Mobility Partner Program enabled us to design a super intuitive user interface that helps clients stay on track with their home exercises a lot better. The proof is in the pudding, with a 2-year study run by the University of Melbourne recently confirming that Physitrack helps to improve client adherence to, and confidence in, their exercise programs when completed via the PhysiApp app. Feedback we receive from clients around the world matches the outcomes of the clinical study, with patients loving the fact they not only have their exercise program and educational content in their pocket, but also can engage with their healthcare provider and provide feedback on their progress. It is no surprise that our built-in Telehealth feature is fast gaining popularity as a way for consumers to ’see’ their trusted healthcare provider. Powered by Dolby Laboratories, clients can have secure video calls with their clinician from inside the PhysiApp client app, enjoying Dolby quality sound and Ultra HD video. A feature clients love especially is the live-streaming of exercise videos, whereby the practitioner can stream any of the Physitrack exercise videos directly to the client’s phone during the Telehealth call. It’s a great way for clients to get a real grasp of the correct technique and be confident they know how to perform the prescribed exercises by themselves. So whether you live in a remote area or enjoy cruising the Greek islands, staying in touch with your clinician is now easier than ever before. Just remember to complete your exercises in PhysiApp before you order your next burger through Uber Eats! Blog post written by Marijn Kortekaas. Marijn is a Partner at Physitrack Ltd. For more information on Physitrack, click here. Disclaimer: This text does not serve as medical advice or an endorsement of a particular product but serves as an example of how technology can improve healthcare. If you have any questions, seek advice from your doctor. Technology is affecting all aspects of healthcare. It is changing how we learn about health, how we monitor our health and also how we treat ourselves. Access to services within healthcare can be hard, especially in the UK. To see a Physio can take many months over here and that is just for the first appointment. Your next appointment can be many weeks later. So when you see your Physio for the first time, they may diagnose you, give you some treatment to help you with the pain and then give you some exercises to help rehabilitate you. But the problem is that you may not be seen or supervised for many months. As a patient you begin to ask yourself whether you are doing your exercises correctly. Who knows? Nobody is monitoring your progress. If only you could access your Physio remotely so that they can let you know whether you are doing things correctly or intervene if there is a problem. Well now you can. Let me explain. About 2 years ago, I went to the gym and did a tough upper body workout. It was a sunny, spring Saturday morning and when I was walking home I noticed that the weeds were growing in the garden. I decided to spend the next 3 hours weeding. I noticed a little niggle in my shoulder but as most men do, I just ignored it and carried on. Over the next week or so the niggle persisted but I carried on life as normal, working, exercising and picking up my 2 year old who never wanted to walk anywhere! Over the course of the next year, this niggle continued. Whenever it started to improve, my 2 year old would develop an aversion to walking and picking him up would aggravate my shoulder. After about 18 months my shoulder started to really hurt. When my wife stated that I reminded her of my young child in that I couldn't get myself dressed, (due to pain rather than laziness!), I felt something needed to be done. Off I went for an ultrasound scan and was diagnosed with Supraspinatus tendinopathy. I then started to get that sinking feeling that anyone with a tendon injury gets ...I've got months of rehab in front of me. I rang Barry Nguyen, (it's very useful when your business partner is also a Physio!) and asked what I needed to do? Don’t stress, was his advice. It will get better but it could take 3-6months. 3-6 months of Physio?!! How much will that cost??!! And I am going to the UK soon, where you can never get an appointment to see a Physio!!! It was then that he introduced me to Physitrack. Physitrack is a way that Physiotherapists can provide you with the exercises that you need to do, monitor your progress remotely and then change your rehab program as needed. So what did I get? I first received an email that showed a series of exercises that needed to be done. The exercises were explained with a clear, short video. I followed the videos. They were painful at first but then they became easy. I sent a message to Barry to let him know of my progress and then I received an email with more exercises to do that were more challenging and so on. The crazy thing was, for a period of time, I was in the UK and Barry was in Australia! After 3 months of intense rehab, I was doing push ups. 4 months, chin ups and 5 months bench press. Don’t get me wrong. I still needed the odd face to face review but most of the rehabilitation was done remotely.
A common complaint that I get as a doctor is that patients are unable to see their Physio often enough. Now with services like Physitrack, you are in communication (electronically) with your Physio who can supervise your recovery remotely, with the safety net of seeing you face to face, if there is a problem. Technology has infiltrated all industries and is slowly being accepted in healthcare. When it can be really hard to access healthcare in first world countries, we as health professionals and patients need to embrace technology to improve the service that we give and receive. Healthcare will never be completely remote but seeing or dealing with a health professional online will become part of the process, along with face to face consultations, when you have a health problem. I had to go to the UK as an emergency and without access to Physitrack my rehabilitation would have been delayed. Instead now my shoulder is better and I much to my wife’s relief, I have finally regained the ability to dress myself again! Blog post written by Dr Khurram Akhter. Khurram is an experienced primary care physician and a thought leader in the field of digital health. Disclaimer: This text does not serve as medical advice or an endorsement of a particular product but serves as an example of how technology can improve healthcare. If you have any questions, seek advice from your doctor. As you have probably noticed, if you have read my blog, I am pretty passionate about health technology. People may ask the question, why? It is a bit of a random topic, so why do I keep going on about how amazing it is? I am passionate because I am surrounded by it at work and can see how it can help people in many ways: it can improve your health, give you better access to healthcare or motivate you to make a change in how you live your life. But allow me to give you a personal example that shows how simple technology can really save lives. I have a family member who is ill. Really ill. Let’s call him Tom. He is 40 years old, has two young boys and has been diagnosed with a brain tumour. At the start of the year, he had a stroke because of the tumour and then spent the next 7 months in the intensive care unit recovering from it. He was unable to talk as he was breathing through a tube in his neck (called a tracheostomy). In spite of the stroke, his tumour was actually stable and not growing, so we got him home. We wanted to get him stronger with rehabilitation and get the tube in his neck out, to get him talking again. Unfortunately he was only granted carers to look after him for part of the day, so the rest of the care was needed to be done by the family. Because of this I set up Tom’s wife, let’s call her Emma, with some basic tech: a blood pressure machine, thermometer and an oxygen monitor and said any problems, call me. One Saturday night, it was 11 o’clock and I got a message from Emma. It was a video of Tom in his bed looking pale and sweaty and breathing very fast. Attached to the video was a note, “Is he ok? Trying to get a doctor, but he won’t be here for at least 4 hours”. I quickly asked her if she could use the blood pressure machine, thermometer and oxygen monitor and let me know the numbers. Blood pressure 109/73, pulse 120, oxygen saturation 84%, temperature 40 degrees. Ok, you budding doctors, what do you think? Can this wait 4 hours or not? With an oxygen level of 84%, Tom would not last 4 minutes let alone 4 hours. My response was to call an ambulance, NOW! She did and Tom was taken to hospital and given treatment for a chest infection. He recovered and returned home to his family within 3 days to continue his rehab. Those who work in health know problems like this always happen late at night, on the weekends when no doctors are available. Now you might say Emma was lucky because she had you to contact if there was a problem. But with the rise of the online doctor, everyone has access to a doctor where and when they need it. In addition, with some objective information in the form of a temperature, blood pressure, pulse rate and oxygen level, the correct decision can be made. There was no need to see him face to face to work out what needed to be done. He needed to go to hospital straight away. Without this information, we would have been guessing what the problem was and probably would have waited 4 hours for a doctor. Had we done that Tom would not have been here today. We are fully aware that he does not have much time with us but because of a bit of simple tech, his two boys get to spend a bit more time with their father, who ultimately will not see them grow up. Whilst this is an extreme example, it shows you why everyone needs a bit of tech in their lives. It really can be the difference between life and death. Blog post written by Dr Khurram Akhter. Khurram is an experienced primary care physician and a thought leader in the field of digital health. Disclaimer: This text does not serve as medical advice and if you have any questions, seek advice from your doctor. There is no doubt that medicine is a complex business. 6 years at medical school gives you the BASIC knowledge to work as a doctor. The next 10 years are focussed on adding to this knowledge and refining your skills. When you reach the “top”, the learning never ends, it just continues as science changes the way we treat people. Your GP or Family Physician has to learn different skills compared to your hospital doctor. When you work in a hospital you have access to blood tests, xrays and scans, the tools to help make a diagnosis. These can be done straight away but most importantly, the results will be back on the same day. In Australia and the UK, your GP can do the same tests but the results will not be back for a few days. So your GP has to decide whether a patient is well enough to wait for a few days for the tests to come back. If they are, the test can be done in the community. If they are not, they must go to the hospital now. Ultimately, your GP is a medical risk manager. What is of interest and may be a bit scary to know is that the physical tools the GP has to make a diagnosis are really quite basic, (we will go into what these are later). Much of the diagnosis is based on the GP’s ability to gather information from the patient by talking to them. They then confirm the diagnosis using the basic tools and decide on a plan based on how urgent they think the problem is. Let me explain in a bit more detail. When someone comes in with a problem such as a cough, I create a list in my head of about 10 things that could cause it. This list starts off with the worst case scenario, eg cancer. It then has the common causes of coughs and then the uncommon causes. Over the years I have learnt about all of the conditions on the list: what symptoms they cause, what you would find if you were to examine someone with the condition, what tests are needed to confirm the condition and how to treat the condition. With years of training I have honed the questions that I ask the patient. With each question a condition gets crossed off or may get added to the list until I have a handful of conditions that I have a strong feeling could be a cause of the symptoms. Once I reach this point I crack open my tool box to examine the patient. I am looking for particular signs that would confirm or disprove the condition that I am considering. This is where it becomes alarming to people out there. As things stand, the tool box I have is really basic. A blood pressure machine, thermometer, a wooden spatula to look in a mouth, a torch to look in an ear and eye, an oxygen monitor, a stethoscope and something to test your urine. That’s pretty much it. Some doctors have a bit more, but not many have less. What it means is that much of your diagnosis is based on your GPs skill and training to get information simply by talking to you. It is the interpretation of what you say and what your doctor finds with very basic tools that determines what your diagnosis is. Ok, that’s all very interesting doc, but what relevance is that to me as a patient? Well if you have those basic tools at home, then you can get your GP to interpret it remotely. The information gathering is mostly done by talking to someone which a GP can do online. If you can provide the information that the doctor would ordinarily get using the basic toolkit in the clinic, then, within reason, you can have a fairly effective consultation. Don’t get me wrong, there are times that you have to see someone in the flesh but much of the time you do not. Many online GP services will have the safety net of organising an in person review if there are ANY concerns. But for health problems that could be dealt with online, if you could provide the same information that would normally be checked in a clinic, you can obtain the nirvana of being able to access a medical review anywhere, at anytime and at YOUR convenience. No need to take time off work or find someone else to look after the kids just to be told, “don’t worry about it. Your cough will settle.” The number of times that I have had patients complain about having to take time off work to see the GP and all they get is reassurance and no antibiotics. I totally understand the frustration and this is why I feel that having the right tools at home and access to an online GP can make the assessment of someone with a health problem more efficient. So what information do I need to provide?
If in addition you have a digital stethoscope then your chest and abdomen can be examined. Add a torch and your throat can be examined. Companies are creating solutions that provide all of these tools in one piece of kit. A company called Tyto Care from Israel is doing this. They are launching in the USA but the UK and Australia must wait. Healthy.io produce a home urine kit that can check for urine infections and kidney problems, (not available in Australia, yet). None of these products are too expensive and for the cost of a big night on the beers, you can obtain a mobile GP clinic. Finally you can start avoiding the frustration that occurs when you have to break your routine to see your notoriously inflexible GP. The GP can do what they do best, which is talk and listen to you. They can guide you through using the necessary tools to obtain the information that they need and make a decision on what the next step will be. Sometimes you will have to come in for an in-person review. Sometimes you won’t. It will be up to the doctor to ensure he or she can make a safe decision with the information to hand. The bottom line is that if you know what information your doctor needs and can give it to them accurately, your life will become so much easier and healthcare will become like most other industries have become, easy to access at a time that is convenient to you. Blog post written by Dr Khurram Akhter. Khurram is an experienced primary care physician and a thought leader in the field of digital health. Disclaimer: This text does not serve as medical advice and if you have any questions, seek advice from your doctor. Recent claims in the media that the “big 4” tech firms (Google, Amazon, Apple and Microsoft) will ‘disrupt healthcare’ are often met with justified expert skepticism. Over the past couple of years, it is with common consensus that these companies do not fully understand the idiosyncrasies of the healthcare industry at an operational level. The provision of healthcare to patients is not a business model that generally fits in with the model of how big tech firms operate and scale. Operating healthcare businesses is generally very local and high touch, requiring relatively high fixed costs and capital investment for lower returns. On various occasions, they have publicly announced their ambitious and ‘disruptive’ healthcare endeavours but with very few making it past the proof of concept.
While big tech will unlikely go into care delivery as a primary priority, they are strongly positioned with their business and technological strengths to play a major supporting role for healthcare provider organisations. The catalyst for this is due to an increasing focus on patient-centred, data driven value based care. This is due to increase in healthcare spending (in the trillions in the US). Big tech see these increasingly healthcare costs as a massive business opportunity. Technology enabled healthcare providers will have a potential competitive advantage and even be a threat to those who provide care under traditional fee for service models. Despite big tech’s capabilities to significantly improve user experiences of clinical information systems and help reduce clinician burnout, it is unlikely that big tech will be able to disrupt this space. The majority of healthcare organisations have heavily invested financial and human resources in current practice management software, and the switching costs to another vendor are astonishingly high. In addition, big tech companies are increasingly not trusted by the public with health data, as a result of recent consumer data privacy and security breaches and government-led antitrust investigations. According to a 2018 US survey by Rock Health, only 11 percent of people were willing to share their health data with a tech company like Amazon or Facebook. Interestingly, the public would rather share their health data with the federal government, insurers and big pharma. Not surprisingly, they are most trusting to share their health data with their doctor. So what are the “big 4” tech firms currently doing in the healthcare space? Google’s primary interests in healthcare appear to be population health, structured data and artificial intelligence. The company is applying artificial intelligence to disease detection, data interoperability and potentially health insurance. Projects include using image processing to screen for diabetic retinopathy, early sign screening for blindness, and early detection of breast cancer via their subsidiary company DeepMind Technologies. In 2014, they acquired DeepMind for a reported $500 million (USD). They have also recently invested $375 million (USD) into a technology focused small health insurer in the US called Oscar Health. They aim to revolutionise health insurance utilising big data and telemedicine. Google AI quotes on their website that they “think AI is poised to transform medicine, delivering new, assistive technologies that will empower doctors to better serve their patients.” Recently, Google DeepMind announced that its artificial intelligence technology can detect acute kidney disease 48 hours before doctors can spot it. This condition is apparently difficult to spot by doctors early as the symptoms and signs are often not clear, leading to potentially fatal kidney injuries including dialysis. Amazon Amazon’s particular strengths are likely their Amazon Web Services (AWS) cloud infrastructure, Alexa AI voice assistant technology and their deep supply chain and delivery capabilities. Amazon have always been interested in healthcare, with its first notable attempt of investing into drugstore.com in 1999. This was an e-commerce play in the pharmacy space which was acquired by Walgreens in 2011 for $409 million (USD) and eventually wrapped up as Walgreens decided to focus on other priorities. Recently, Amazon acquired an online pharmacy called PillPack for $753 million (USD) and later announced a partnership with JPMorgan Chase and Berkshire Hathaway, to develop an independent healthcare company to look after their US employees and associated family’s health, with the goal of improving employee satisfaction and reducing costs. Apple Apple’s strength is in consumer facing products. The big tech company successfully secured one of the 9 exclusive spots in Food and Drug Administration’s (FDA) Digital Health Pre-Certification Program. This program run by the US government evaluated applicants for their robustness and quality control protocols, to certify them for the development of future medical technologies. Apple is also involved in many university research collaborations but notably, the Apple Health Study with Stanford University. This study utilises the Apple Watch’s heart rate sensor to collect data on irregular rhythms and alert users who may be experiencing the heart condition atrial fibrillation. In 2018, Apple signalled the entrance into the electronic health record space by launching HealthKit API. An Application Programming Interface (API) simply allows independent software applications to talk to each other with certain defined constraints. This enables users to share their clinical and personal health data with developers via trusted smartphone third party apps. Apple have also entered the healthcare payment space with their solution Apple Pay with recently announcing their partnership with US health insurance company UnitedHealthcare. Microsoft Microsoft have focussed their resources on their trusted healthcare IT infrastructure through solutions such as Azure (like Amazon Web Services) and big data analytics capabilities to advance precision medicine. Precision medicine is "an emerging approach for disease treatment and prevention that takes into account individual variability in genes, environment, and lifestyle for each person." (Precision Medicine Initiative). In 2017, Microsoft setup a healthcare division at a Cambridge University research facility in the United Kingdom. The work at this research lab focuses on the application of big data, artificial intelligence, machine learning and cloud computing on healthcare problems. Microsoft’s healthcare division boasts a multi-billion dollar resource with claims to have over 1,100 employees, 168,000 customers and 14,000 partnerships. Final thoughts The “big 4” tech firms are already playing a critical role in influencing the healthcare industry globally, and this will be even more prominent over time with the pressing focus on value based healthcare. Products and solutions from such companies will increasingly become more distributed and sophisticated as technology and the quality and volume of data improves. Nonetheless, they also have some key immediate challenges, which is firstly to win over consumer trust with their solutions, where data privacy and security concerns are of greatest importance to clinicians and their patients. It will be interesting to see over the next decade in regards to how healthcare will be transformed by technology, and how the big 4 tech firms will collaborate with the industry while supporting startups and new innovations. Optimistically, we will see as a byproduct, a significant improvement in quality of life of all stakeholders including clinicians, patients, researchers and administrators. Truly exciting times ahead of us. Disclaimer: This text does not serve as medical advice and if you have any questions, seek advice from your doctor. Blog post written by Barry Nguyen, an experienced sports and musculoskeletal physiotherapist and digital health expert. Background on low back pain
Low back pain is a very common health condition worldwide and a major cause of disability in all age groups. It can impact the level of functioning at work and life in general. The economic impact of lower back pain in the United State of America has been estimated to be over 100 billion dollars annually and growing. Lower back pain can be classified as acute (less than 6 weeks), sub-acute (6 to 12 weeks) or chronic (> 12 weeks). Low back pain symptoms Low back pain is generally not considered a ‘disease’ but a group of symptoms which may include:
Causes of low back pain In most cases, the cause of low back pain is unknown or difficult to pinpoint but multiple risk factors have been identified contributing to the development of lower back pain which include:
Popular medical management of low back pain Radiological imaging such as x-rays, CT scans and MRIs of the lumbar spine are often unreliable and unhelpful in determining the cause of your lower back pain. Popular medical treatments include pain killers (analgesics) and anti-inflammatories despite a lack of scientific evidence associated with its efficacy carrying potential side effects, as the causes of lower back pain are rarely addressed. Preferred evidence based treatment options include physical therapy (physiotherapy), joint mobilisation and manipulation, exercise rehabilitation, cognitive behavioural therapy and pain re-education. Surgical intervention is generally the least preferred option, and considered when conservative non-invasive management fails. When to seek medical attention? It is important to note that back pain can be a signal to a very serious medical condition so please seek immediate medical attention if you experience symptoms including:
Some tips to prevent low back pain or recurrence
Innovative tools which can help your back pain There are many tools available in the market that can help monitor and manage your lower back pain. There is an increasing number of innovative solutions in the market which promote drug free pain relief of your lower back pain including PainPod and Quell. There are also wearable devices which help improve your posture and core muscles at work and at home, notably, UprightGo. There are many exercise rehabilitation apps which assist in providing exercise programs to prevent and rehabilitate lower back pain conditions for example, Kaia’s back pain app, which in a recent study, demonstrated that it was more effective than traditional therapy and online education. Using wearables or activity trackers such as Fitbit, Garmin, Apple’s step counter, Strava or RunKeeper apps can help with behavioural change and promote good exercise habits. Disclaimer: This text does not serve as medical advice and if you have any questions, seek advice from your doctor. Blog post written by Barry Nguyen, an experienced sports and musculoskeletal physiotherapist and digital health expert. The workshop, organised by the Australian Digital Health Agency, brought together experts and key groups at the Brisbane Convention and Exhibition Centre. The purpose of the workshop is to address the challenges of health apps and discuss how to ensure they are evaluated to benefit patients. Key groups included the Therapeutic Goods Administration, the Australian Commission on Safety and Quality in Health Care, Consumer Health Forum, CSIRO and Queensland Health.
The key questions that were considered for the workshop were:
Privacy and security of the data was the primary challenge associated with mHealth apps given it is a complex area to manage and resolve with all stakeholders. There was a key discussion about the consumer perspective and it was noted that based on a small survey of consumers, they view that GPs are the most trusted source when it comes to health app recommendations. However, this poses the question of whether GPs are sufficiently trained to evaluate and recommend health apps. Consumers also want to know who funds mental health apps as well as who endorses it. This feedback will likely apply to other clinical specialities such as physiotherapy modalities. Other particular challenges associated with mHealth include:
There needs to be transparency and informed consent regarding the secondary use of the data and how it is managed, including the risks. In terms of providing an opinion or endorsement for an app, there were questions asked:
In conclusion, there appeared to be a group consensus that a national framework for health apps needs to be developed and the Australian Digital Health Agency needs to lead the charge with collaborators. So what does this mean for physiotherapists? The clinical application of mHealth is an increasingly relevant area given the amount of physiotherapy-related apps that are in the market and its easy accessibility to our patients. As clinicians, it is important to be informed and be aware of the benefits versus the risks of such solutions, including what would happen to your patient data, privacy and security concerns, as well as the emerging research associated with particular solutions. At this stage, your first priority should be to ensure that what you may recommend, or are aware of what your patients are using, is safe and has a potential value to their health. Disclaimer: This text does not serve as medical advice and if you have any questions, seek advice from your doctor. Blog post written by Barry Nguyen, an experienced sports and musculoskeletal physiotherapist and digital health expert. The “Quantified Self” movement is here. This movement is associated with individuals utilising technology such as wearable devices and mobile phone apps to track specific health parameters (mental, emotional, physical and social) in their daily lives. The collection of daily data can help the individual gain self-knowledge to improve their quality of lives through potential actionable insights such data can provide. With the emergence of health consumerism and advancements in technology, there is an increasing number of relatively inexpensive wearable devices and mobile phone apps which enable individuals to track various health parameters during their daily lives, including symptom logging, sleep hygiene, stress levels, heart rate, diet and activity levels. There is an increasing amount of physical products available to the public at retailers from popular brands such as Apple, Samsung, Garmin, Fitbit and Polar. There are also more advanced niche products such as the Athos Training System, which is a smart garment which tracks muscle activity and motion. All of these products have broader implications for physiotherapists when managing their patient’s general health and optimising clinical outcomes. Health professionals such as physiotherapists are traditionally guided by established science and evidence based practice guidelines. Therefore, the self-quantification movement may seem in conflict with this due to the experimental nature of this approach and relatively smaller population sizes applied. Nonetheless, there is an increasing number of health professionals such as physiotherapists who are looking more closely at how to extract meaningful insights from this data from self-tracking to optimise health outcomes at both an individual and population level. In particular, many of the measures from such solutions can assist physiotherapists in behavioural change and promoting healthier lifestyles. Key factors that have contributed to the rise of self-quantification and self-experimentation include:
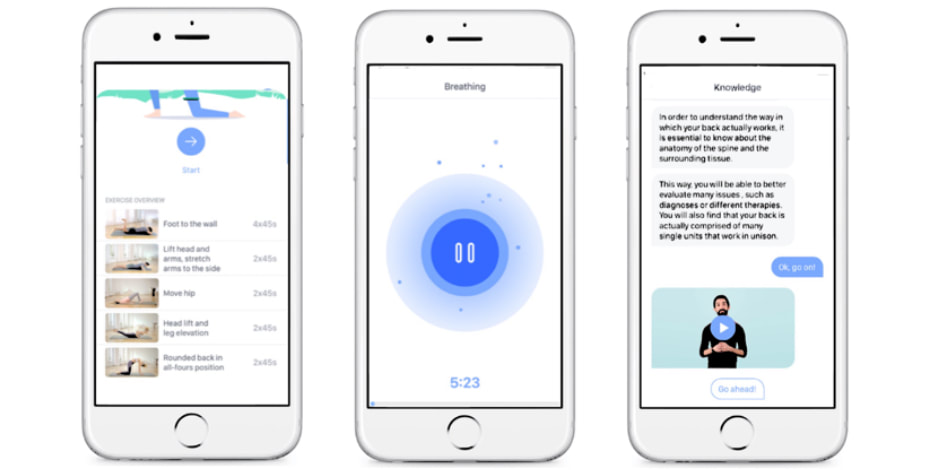
What are the implications for physiotherapists managing patients who are self-quantifiers? From one perspective, self-quantifiers are ideal patients as they are engaged and proactive in taking responsibility over their own health. However, it is important to be aware that being unprepared for such scenarios can result in patients challenging the physiotherapist’s knowledge, and as a result, threaten their authority. So in such circumstances, it may be best for the physiotherapist to take a strong collaborative and work with the patient as partners in their health, focusing on helping their patient achieving their goals, ensuring that the patient is informed of the potential benefits and risks associated with what they are experimenting with, and ensure avoiding any potential danger and safety issues. An example of self-quantification often used in the community are activity tracking solutions such as the Strava app, Fitbits, Apple and Garmin watches. This has been reported to be a useful tool for physiotherapists as it can provide insights into external training load and assist with injury prevention and performance optimisation. In addition, the online social community associated with many of these apps which often incorporate benchmarking performance can be helpful for motivation and support. A back pain app outperforming physiotherapy? With an increasing number of freely available articles on the internet such as “The back pain app out-performing physiotherapy” backed by a randomised control trial, physiotherapists should start to take serious note of the longer term implications of how emerging digital health solutions may impact their practices and patients. Without going into the details of the limitations of this study, it recently demonstrated that patients using the Kaia app reported significantly less pain than the control group which comprised of weekly physiotherapy and online education. Both groups were encouraged to incorporate an active lifestyle and perform a home exercise program. The Kaia app comprises of 3 therapy modules: back pain education, hands off physiotherapy, and mindfulness/relaxation techniques. Users of the app also have the ability to interact with a human coach via the app if they have any particular questions. This study adds to the emerging body of evidence which supports a “multi-modal approach” to chronic pain management. Traditionally, multi-modal treatment approaches to chronic pain management is often costly, limited to a small number of specialised medical facilities and appropriate clinical team. The results of this study provide promise that emerging digital health technologies have the potential to provide viable alternatives to traditional models of care, providing better accessibility, affordability and in many cases, more effective treatment solutions for specific populations. Key implications for physiotherapists:
Disclaimer: This text does not serve as medical advice and if you have any questions, seek advice from your doctor. Blog post written by Barry Nguyen, an experienced sports and musculoskeletal physiotherapist and digital health expert. Chatbots are becoming commonplace in society, and are often used for virtual assistance, marketing, customer support and technical troubleshooting. This technology is emerging in healthcare with many startups in this field which include patient symptom checking and triaging, pre-consultation history taking and even assisting patients with common mental health conditions. The most popular chatbots currently in the market include virtual assistants such as Google Home and Amazon Alexa, and via messaging apps such as Facebook messenger, Whatsapp, WeChat and independent website landing pages.
So what exactly is a chatbot? A chatbot is software or a combination of software and hardware, enabled by varying levels of artificial intelligence which can conduct a conversation with a human user via auditory or textual approaches. They are designed to simulate as close as possible to human conversational behaviours. Potential Benefits
Risks and Limitations
Application in Physiotherapy There is an increasing number of use cases for physiotherapy and chatbots. As the chatbot technologies improve, this will continue to increase. There are a number of emerging chatbot solutions that the physiotherapy industry are incorporating for:
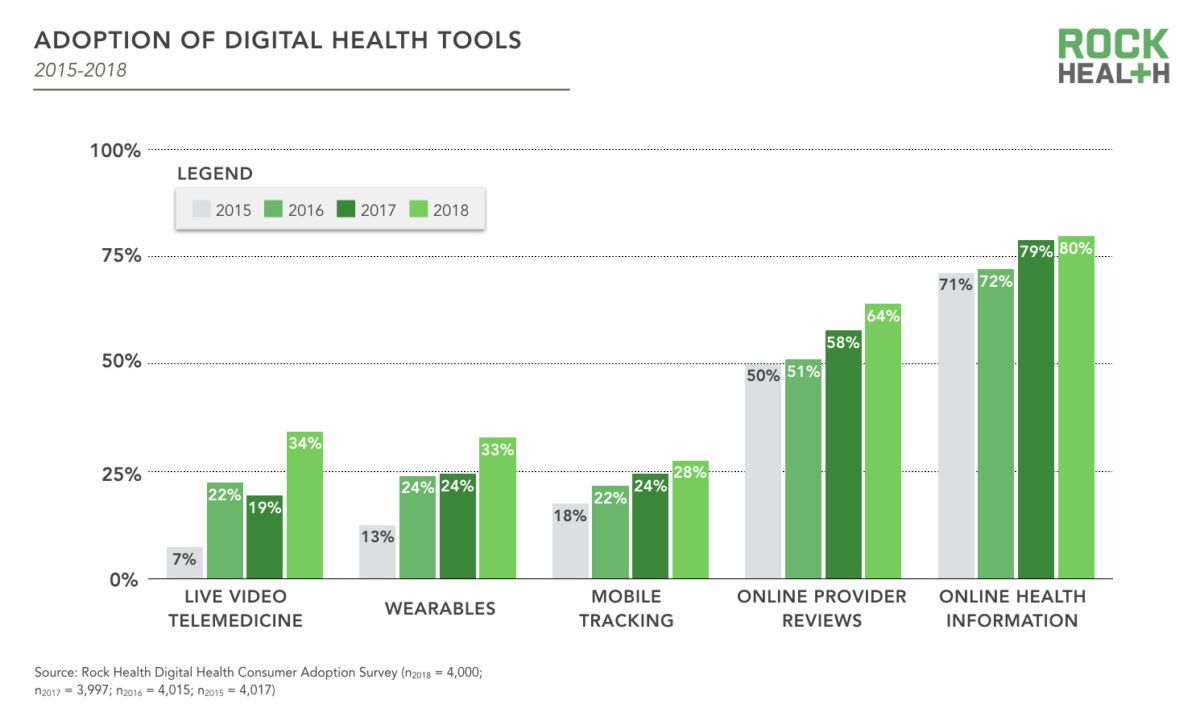
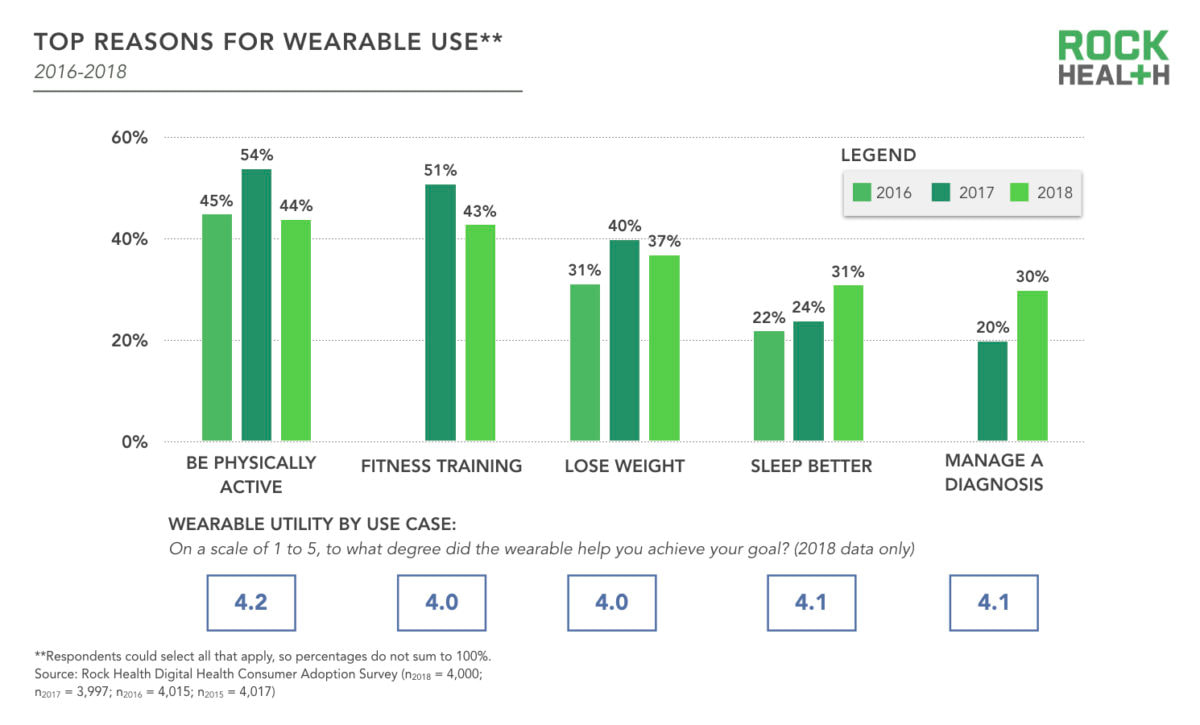
The Future As chatbot technologies become more mature and sophisticated, we will likely see more solutions in the market that can provide new value to physiotherapists and their patients. This will most likely begin with a surge of solutions, assisting physiotherapists with administrative burdens through intelligent automation. Artificial intelligence and machine learning powered solutions also have the potential to support physiotherapists with practitioner-patient communications, data collection, clinical decision making, symptom checking, health coaching, and patient triaging. The future is bright as such solutions will enable physiotherapists to focus on more complex work and patient care. Recently, Amazon in the US announced that its virtual voice assistant Alexa will be HIPAA compliant and conducting pilots in the healthcare space. Via voice recognition, this will enable consumers to do tasks such as making appointments with their doctors, and even access post-discharge instructions from their hospital. Yes, chatbots are likely to kill menial jobs in the longer term but will likely produce new ones that allow humans to be more productive, creative and ultimately, add more value to the world. Disclaimer: This text does not serve as medical advice and if you have any questions, seek advice from your doctor. Blog post written by Barry Nguyen, an experienced sports and musculoskeletal physiotherapist and digital health expert. Rock Health, a leading US venture fund devoted to supporting and investing in digital health startups recently released a report from a 2018 consumer survey on digital health adoption and sentiments. Comparing the latest results from consumer surveys from previous years, there appears to be a shifting trend from interest in low risk entry digital tools that assist with fitness and wellness towards those that assist with managing health conditions - “with the intention to address concrete health needs”. It is important to note these tools often do not reach those who are in need of it the most. Technology adoption has generally been a challenging task with rural, disabled and elderly populations. These populations often have poor digital literacy, access to the internet and relevant hardware (such as smartphones and computers). Nonetheless, there are an increasingly number of exciting startups that make digital health tools easier to use and more accessible for these populations. In the survey, digital health tools were grouped into 5 different categories:
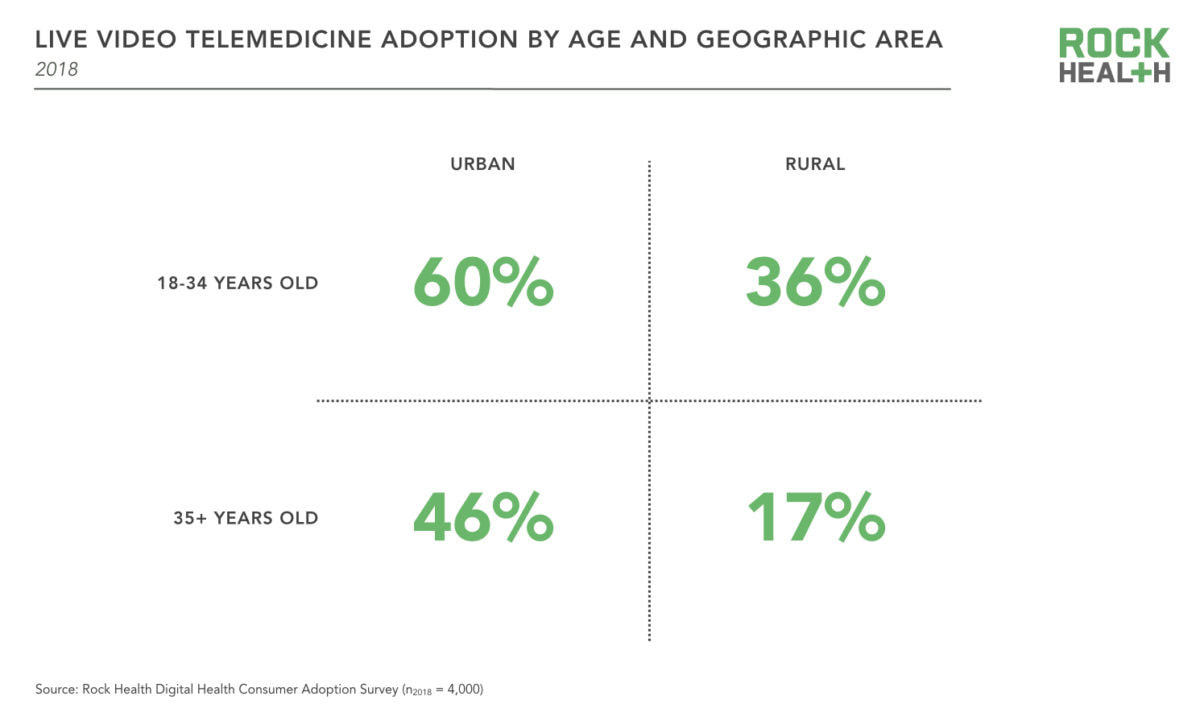
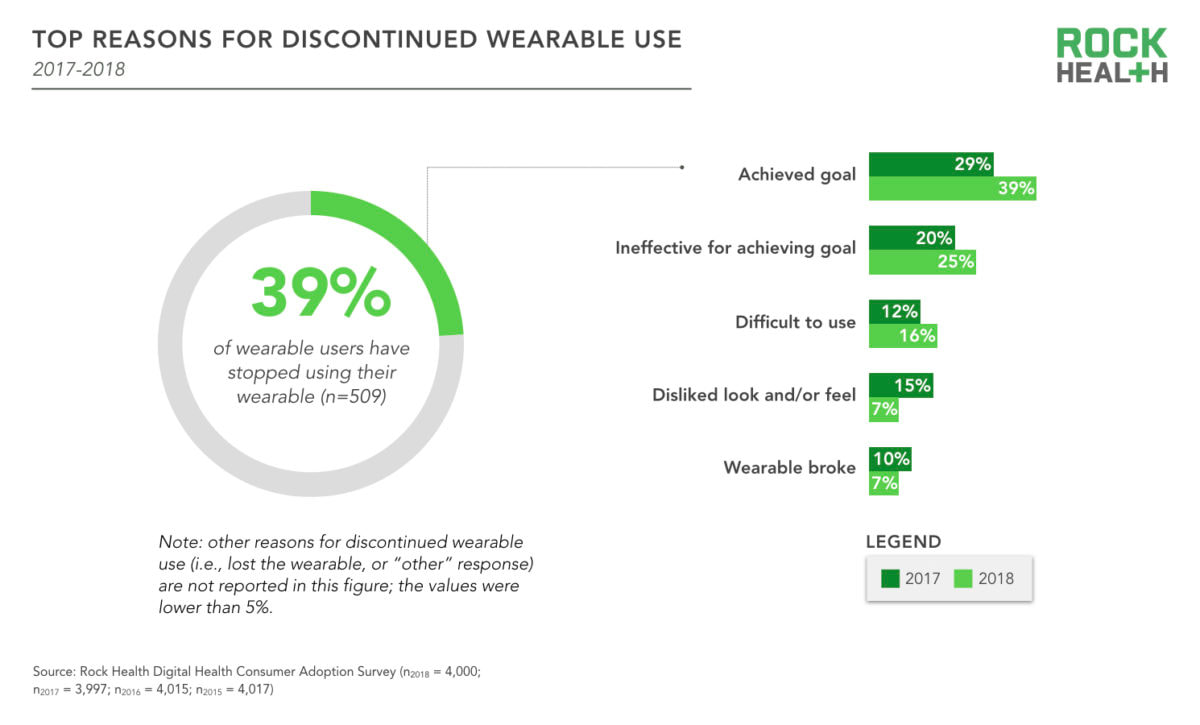
As the graph illustrates below, there is a continued increase over the past 3 years in the adoption of digital health tools and services related to these 5 categories. More interestingly, despite the leading use of wearables is for physical activity, survey respondents are demonstrating a shift towards using wearables from fitness and well-being towards managing diagnoses with potential clinical relevance to health professionals. This trend suggests that healthcare providers will increasingly need to be aware of the emerging consumer use and inquiry of these tools, as the data collected from such devices can potentially assist health professionals in providing patients with further insights into their condition. Another interesting trend is urban consumer adoption of telemedicine services is more than twice as likely than rural consumers. Not surprisingly, tech savvy millennials are the target market of many of these telehealth startups, who are seeking convenience in engaging in healthcare services like the way they engage in food delivery and transportation services. There are also 2 major issues to note that potentially stifle consumer digital health adoption. They are notably privacy and security concerns, and the discontinued use of such tools. There is an increasingly public distrust in sharing personal health data with large tech companies due to a number of scandals which includes the highly publicised Facebook-Cambridge Analytica drama. Health professionals (notably, physicians) remain the most trusted by the public in relation to confidence in sharing personal health data. The survey also identified the leading reasons associated with the discontinued use of wearable devices. It is important for health professionals to be aware of the common reasons which include:
Some key implications from the survey results:
Disclaimer: This text does not serve as medical advice and if you have any questions, seek advice from your doctor. Blog post written by Barry Nguyen, an experienced sports and musculoskeletal physiotherapist and digital health expert. There is emerging scientific research that training loads are directly correlated to injury risk. Training load injuries are generally caused by:
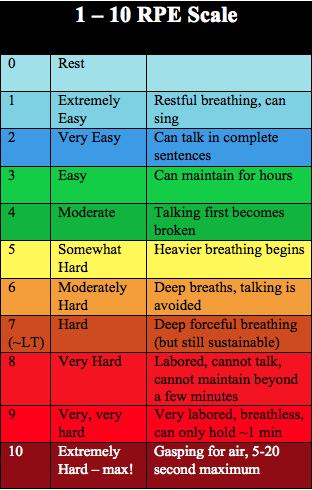
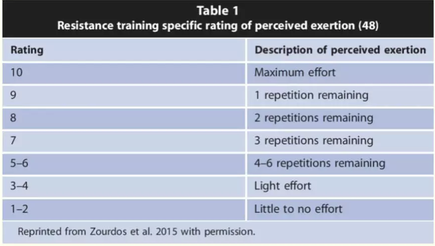
External vs Internal Training Loads Specifically, there are 2 types of training loads: External Loads and Internal Loads. External loads measure the amount of external workload eg. (running on the treadmill, weight lifting) to the individual while internal load measures the individual’s post exercise heart rate or rate of perceived exertion (RPE) as a response to the external workload. Rate of Perceived Exertion Guides for Aerobic and Resistance Training It is important to understand that to optimise performance, there needs to be a fine balance between training hard and overloading resulting in injuries and comprising performance. This sounds like common sense however to accurately monitor training loads is a challenging task given that it is associated with frequency, duration and intensity. Duration and frequency are relatively easy to measure however intensity could be measured by for example, how fast you are running, your heart rate, how much weight you are lifting with the barbell or the complexity or speed of the movements you are performing. Tracking your training loads is not just about managing the specific exercise you are doing but can help you determine when it may be appropriate for you to do some cross-training or vary your load. Acute on Chronic Workload Ratio (ACWR) For those who are a serious about injury prevention and performance optimisation,a great way to find your training ‘sweet spot’ while minimising the risk of injury is by using the Acute on Chronic Workload Ratio calculator. Scientific research indicates a 0.8-1.3 ratio range is ideal. Injury risk increases at a 1.5 ratio or higher. To calculate your ratio, multiply your rate of perceived exertion (RPE) after each exercise with the duration, intensity or frequency of the exercise session (external load). The Acute Workload is over a 7 day period. The Chronic Workload is over a 28 day period. The ratio is the result of dividing the Acute Workload by the Chronic Workload. Tips:
Disclaimer: This text does not serve as medical advice and if you have any questions, seek advice from your doctor. Blog post written by Barry Nguyen, an experienced sports and musculoskeletal physiotherapist and digital health expert. Asthma is common. It can make you pretty sick and limit your ability to work, exercise or do daily activities. Colds and other lung problems can cause your asthma to worsen rapidly, so it is important to know that your asthma is well controlled and be able to identify when things are going wrong. Background A bit of background on asthma. Imagine you have a series of pipes in the lungs that enable air to travel in and out. With asthma, things like dust, pollen, viruses or exercise can make those pipes become narrow, preventing as much air from travelling in and out. You will then develop symptoms of shortness of breath, wheezing or a cough. As you can imagine a severe attack can make you very unwell, as you cannot breathe. Emergencies When diagnosed with a long term health condition, it is important to know what to do in the worst case scenario. How to recognise a problem, how to act and when to call for help. It is vital that you learn this or be able to access the necessary information quickly. Downloading the Australian Red Cross First Aid app on your phone will give you a resource that you can refer to whenever you need. (Remember if in doubt, call the emergency services). Avoiding Triggers Of Your Asthma Understanding your environment is important if your asthma is triggered off by pollen or pollutants. Having data that tells you that the air quality is poor may remind you to take your inhaler just in case. Or maybe you should take the train today rather than cycle. An air pollution monitor can provide valuable insights into whether your asthma may be triggered today or not. Tools To Identify If Your Asthma Is Worsening
Knowing how to identify a problem early before it makes your asthma worsen is vital. You can do this by having the right tools at home that can give you clear information on the health of your lungs or signs of infection. Oxygen monitors, thermometers, digital stethoscopes and blood pressure machines should be part of your new first aid kit. They will give you key information as to whether you need to see a doctor or not. In addition, if you access an online GP, the information these tools provide will enable the doctor to provide a safe and thorough assessment. As a result, you can seek medical advice quickly at a time and place that is convenient to you. Our list of favourites is not exhaustive and we encourage you to look at other products on the website and see what else may be of use. What we are aiming to achieve at HealthAide is that you are able to make an informed decision when considering what else can keep you healthy. New products and services are coming out that will help you manage your asthma and access healthcare quickly. As technology develops so will your ability to reduce the impact of any health issue on the quality of your life. Blog post written by Dr Khurram Akhter. Khurram is an experienced primary care physician and a thought leader in the field of digital health. Disclaimer: This text does not serve as medical advice and if you have any questions, seek advice from your doctor. How we access healthcare varies from country to country but rarely do you find patients content with the service they receive. In the UK the service is free yet you may have to wait 2-4 weeks to see your primary care physician for a non urgent consultation. In the USA, costs are excessive. These issues lead to poor standards of health within the population. Advances in technology (digital health), however mean that this no longer needs to be the case. But how can we use digital health to our advantage? In an age where we like to be in control of most things in our lives, we need to start taking control of our health. Doctors are given ownership of our health but rarely have the time to focus on in depth holistic care. In an age where information is everywhere, we can educate ourselves on healthier living but care must be taken in choosing where that information comes from. We can track many health parameters using our watches etc but which parameters are really of use: the number of steps you have walked or your heart rate? Also is this information accurate? Having learnt about your health and recorded relevant information, it is important to have a professional interpret it, but how can you obtain an appointment quickly and cost effectively? Now that you have found a professional to talk to, do they have the expertise and understanding of the developments in medicine, to analyse your data and then tailor your care to your own personal biology? The benefits of digital health are reliant on 4 pillars:
We at HealthAide.co are creating an environment where motivated individuals can improve their health using the 4 pillars of digital health.
Healthcare is a heavily regulated industry that is not meeting the needs of the population irrespective of whether the patient is paying for their care or not. We need to alter our mindset as doctors and patients and only then will standards improve. We both need to embrace the pillars of digital health and in time this will ultimately improve standards of our health wherever we are. Blog post written by Dr Khurram Akhter. Khurram is an experienced primary care physician and a thought leader in the field of digital health. |
AuthorContributors Archives
March 2020
Categories
All
|
|
SOCIAL
|
HealthAide is an independent resource. We do not own shares or make profits from the products listed on this site. Products and services have been curated using the Four Principles of Healthcare Ethics (Beauchamp, T. and Childress, J. (1985) Principles of Biomedical Ethics)
© COPYRIGHT 2018. ALL RIGHTS RESERVED.


























 RSS Feed
RSS Feed